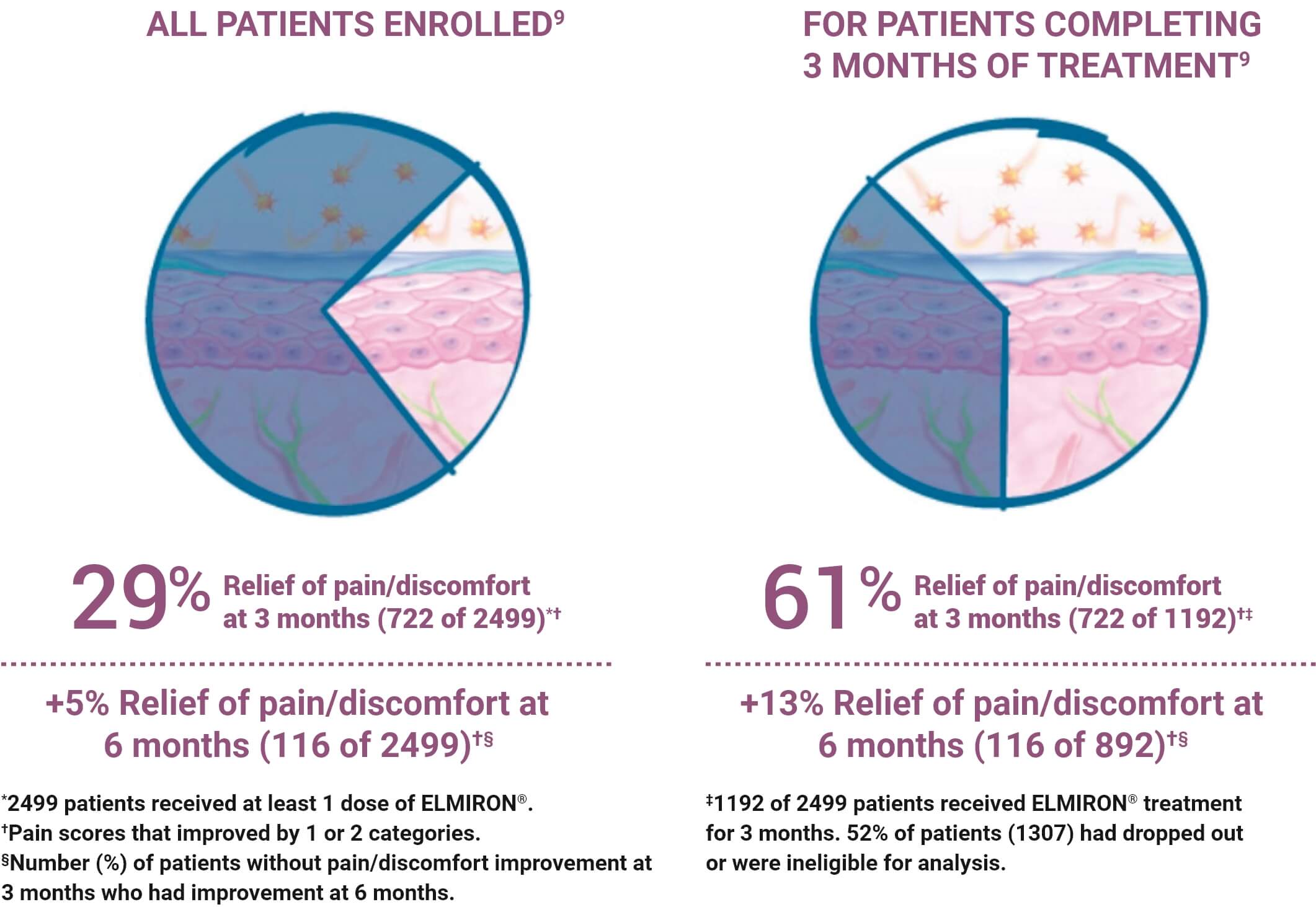
ELMIRON® (pentosan polysulfate sodium) may provide symptom relief in as soon as 3 months8
Since there was not a control group of patients with interstitial cystitis who were concurrently evaluated, it is difficult to determine which events are associated with ELMIRON® and which events are associated with concurrent illness, medicine, or other factors.
| Body System/Adverse Experience | ELMIRON® n=128 | Placebo n=130 |
|---|---|---|
| Central Nervous System Overall Number of Patients* | 3 | 5 |
| Insomnia | 1 | 0 |
| Headache | 1 | 3 |
| Severe Emotional Lability/Depression | 2 | 1 |
| Nystagmus/Dizziness | 1 | 1 |
| Hyperkinesia | 1 | 1 |
| Gastrointestinal Overall Number of Patients* | 7 | 7 |
| Nausea | 3 | 3 |
| Diarrhea | 3 | 6 |
| Dyspepsia | 1 | 0 |
| Jaundice | 0 | 1 |
| Vomiting | 0 | 2 |
| Skin/Allergic Overall Number of Patients* | 2 | 4 |
| Rash | 0 | 2 |
| Pruritus | 0 | 2 |
| Lacrimation | 1 | 1 |
| Rhinitis | 1 | 1 |
| Increased Sweating | 1 | 0 |
| Other Overall Number of Patients* | 1 | 3 |
| Amenorrhea | 0 | 1 |
| Arthralgia | 0 | 1 |
| Vaginitis | 1 | 1 |
| Total Events | 17 | 27 |
| Total Number of Patients Reporting Adverse Events | 13 | 19 |
| * Within a body system, the individual events do not sum to equal overall number of patients because a patient may have more than one event. | ||
The adverse events described below were reported in an unblinded clinical trial of 2499 interstitial cystitis patients treated with ELMIRON®.9
Frequency (1 to 4%): Alopecia (4%), diarrhea (4%), nausea (4%), headache (3%), rash (3%), dyspepsia (2%), abdominal pain (2%), liver function abnormalities (1%), dizziness (1%).
Frequency (≤ 1%):
Digestive: Vomiting, mouth ulcer, colitis, esophagitis, gastritis, flatulence, constipation, anorexia, gum hemorrhage.
Hematologic: Anemia, ecchymosis, increased prothrombin time, increased partial thromboplastin time, leukopenia, thrombocytopenia.
Hypersensitive Reactions: Allergic reaction, photosensitivity.
Respiratory System: Pharyngitis, rhinitis, epistaxis, dyspnea.
Skin and Appendages: Pruritus, urticaria.
Special Senses: Conjunctivitis, tinnitus, optic neuritis, amblyopia, retinal hemorrhage.
Pigmentary changes in the retina, reported in the literature as pigmentary maculopathy, have been identified with long-term use of ELMIRON®. As these reactions were reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
The Physician’s Usage Study is a prospectively designed, open-label, retrospective analysis of 2499 patients who received ELMIRON® (pentosan polysulfate sodium) 300 mg/day.
Patient’s pain/discomfort scores were evaluated every 3 months.
The endpoints of the study were the patient rating of overall change in pain from baseline and the change in pain/discomfort score from baseline.
In a separate, blinded, randomized, placebo-controlled study (N=151), 38% (28/74) of patients taking ELMIRON® 300 mg/day reported a greater than 50% improvement in bladder pain at 3 months compared with 18% (13/74) of patients taking placebo (P=0.005).9
ELMIRON® is an oral medication taken 3 times daily
(Each capsule contains 100 mg of ELMIRON®)
Take ELMIRON® with water least 1 hour before meals or 2 hours after meals
Counsel patients to continue their ELMIRON® therapy
Clinical response may require 3 to 6 months of continuous therapy
Patients may need to stay on ELMIRON® therapy for several months, even if relief is not immediate
ELMIRON® must be taken continuously as prescribed for relief
If improvement has not occurred and if limiting adverse events are not present, ELMIRON® may be continued for another 3 months.
Discussing this with patients from the start of therapy is important.
The clinical value and risks of continued treatment in patients whose pain has not improved by 6 months are not known.
Please see full Prescribing Information for ELMIRON®.
Avoiding foods that have been reported to trigger symptom flares in IC patients may help provide symptom relief.
Tell your patients to track and avoid irritating foods or beverages that affect symptoms.
Click to download the to help support your patients in making “IC-smart” meal choices.
Patients can manage stress-induced symptom exacerbations through techniques such as:
Controlled breathing exercises1
Applying warm or cold compresses on the lower abdomen10
Physical therapy (eg, gentle stretching and pelvic floor muscle relaxation)1-10
Bladder training - practice scheduled voiding patterns to gradually increase time between voids1
References: 1. U.S. Department of Health and Human Services. Interstitial cystitis/painful bladder syndrome. Accessed June 6, 2022. https://www.niddk.nih.gov/health-information/urologic-diseases/interstitial-cystitis-painful-bladder-syndrome 2. Butrick CW. Patients with chronic pelvic pain: endometriosis or interstitial cystitis/painful bladder syndrome? J Soc Laparoendosco Surg. 2007;11(2):182-189. 3. Metts JF. Interstitial cystitis: urgency and frequency syndrome. Am Fam Physician. 2001;64(7):1199-1207. 4. Dell JR, Mokrzycki ML, Jayne CJ. Differentiating interstitial cystitis from similar conditions commonly seen in gynecologic practice. Eur J Obstet Gynecol Reprod Biol. 2009;144(2):105-109. 5. Myers DL, Aguilar VC. Gynecologic manifestations of interstitial cystitis. Clin Obstet Gynecol. 2002;45(1):233-241. 6. Dason S, Dason JT, Kapoor A. Guidelines for the diagnosis and management of recurrent urinary tract infection in women. Can Urol Assoc J. 20011(5):316-22. 7. Hummelshoj L, De Graaff A, Dunselman G, et al. Let's talk about sex and endometriosis. J Fam Plann Reprod Health Care. 2014;40(1):8-10. 8. Fariello JY, Moldwin RM. Similarities between interstitial cystitis/bladder pain syndrome and vulvodynia: implications for patient management. Transl Androl Urol. 2015;4(6):643-652. 9. ELMIRON® [Prescribing Information]. Titusville, NJ: Janssen Pharmaceuticals, Inc. 10. Hanno PM, Erickson D, Moldwin R, et al. Diagnosis and treatment of interstitial cystitis/bladder pain syndrome: AUA guideline amendment. J Urol. 2015;193(5):1545-1553.